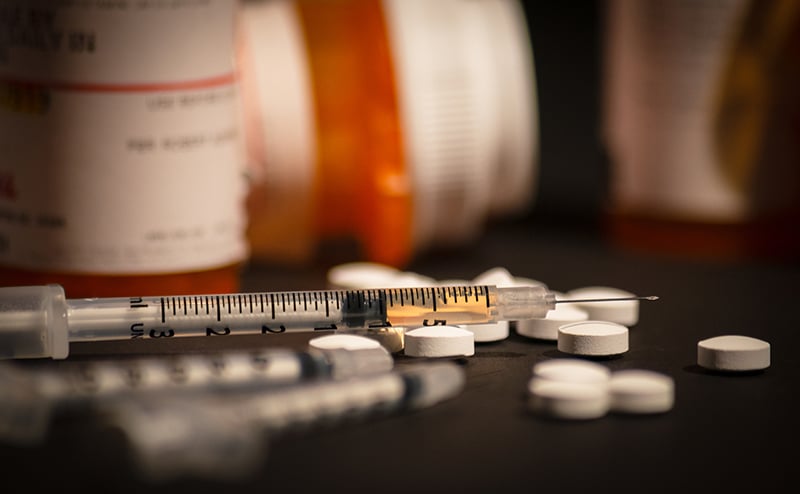
WASHINGTON, D.C.—August 31 marks International Overdose Awareness Day, and unfortunately the COVID-19 pandemic has complicated treatment and recovery for many people who struggle with substance use disorder and opioid misuse. Recognizing the signs of a drug overdose and knowing what to do could save a life, according to the American College of Emergency Physicians (ACEP).
“Drug overdose emergencies are not on hold just because we are in the middle of a pandemic,” said William Jaquis, MD, FACEP, president of ACEP. “In fact, reports show that overdoses are sending an increasing number of people to the emergency department over the last several months. You can save a life by recognizing the warning signs or knowing what to do if you encounter somebody who has overdosed.”
For patients and families, it is important to recognize the signs of an opioid or other kind of drug overdose:
- Small, constricted pupils
- Falling asleep or loss of consciousness
- Slow, shallow breathing
- Choking or gurgling sounds
- Limp body or extremities
- Pale, blue, or cold skin
- Significant changes to vital signs (drastic rise or drop in temperature, weak or rapid pulse, rapid or slow heartbeat)
- Nausea, vomiting, diarrhea
Like all medical emergencies, timing is critical, and it is best to call 911 without hesitating. While speaking to a 911 operator or waiting for emergency medical help, try to keep the person awake and take steps to make sure they can breathe, such as laying them on their side, or in some cases, administering CPR. Stay with the person until emergency medical professionals arrive.
Emergency physicians are concerned that overdoses are increasing with incidents nationwide up 18 percent in March, 29 percent in April and 42 percent in May, compared with the same months in 2019, according to the Overdose Detection Mapping Application Program, a federal initiative that collects data from ambulance teams, hospitals and police. In June 2020, a Centers for Disease Control and Prevention (CDC) analysis showed that 40 percent of American adults reported struggling with mental health or substance use.
ACEP is working to enhance access to emergency care and reduce stigma among those who suffer from substance use disorders, including Opioid Use Disorder. In addition to advocating for more collaborative care—inside and out of the emergency department— which can improve treatment and prevention efforts in communities nationwide, ACEP is working with regulators and policymakers to make sure that patients can be treated for an overdose in real time with naloxone by anyone who is shown how to use the lifesaving Opioid reversing agent. Following care for an overdose, the patient can be treated with Medication Assisted Treatment administered by an emergency physician and will have follow-up care arranged.
Many emergency departments are pursuing accreditation in pain management through the ACEP Pain and Addiction Care in the Emergency Department (PACED) program. Accredited emergency departments meet best-in-class standards for treating pain and addiction while minimizing the use of opioids or in some cases prescribing alternatives to opioids.
“Unfortunately, many people lack a critical support system outside of the emergency department to begin with, whether due to limited local resources or other barriers to access. Emergency physicians are protecting patients by closing gaps in care. The reality is that an emergency physician could provide the only medical attention that many vulnerable people receive during these challenging times,” said Dr. Jaquis.
 American College of Emergency Physicians
American College of Emergency Physicians